‘Digital Twins’ is a concept used in multiple industries. It’s where the physical world is represented in a digital environment to enable a way to view events in real time and provide insights after they happen.
With ambulance service demand increasing, optimising operations to support patient care is more critical than ever. Ambulance authorities now need to deliver more services with fewer resources in an ever-changing environment, and often rely on outdated legacy systems that are largely manual and disconnected.
This is where Digital Twins can help. They are used right now in the health space to support next-generation models of care – delivering truly integrated patient treatment, and dramatically increasing prehospital efficiencies and effectiveness like that achieved by the South Central Ambulance Service in the United Kingdom.
This blog examines the Digital Twins concept and the future of integrated patient care information. It also shows how connecting clinicians and data to support patient outcomes delivers truly integrated and collaborative patient care.
What’s the Current Situation with Prehospital Data?
We’re in a glut and experiencing the compounding effects of too much (disconnected) data. The ability to properly capture and understand, let alone analyse and comprehend the large volumes of information generated is overwhelming. While there is so much information available, it feels like there isn’t enough.
This is due to multiple scenarios, including:
- Standalone solutions often delivered to fix a problem in the short term. “We need it right now, and we’ll worry about integration later.” For example, an Excel spreadsheet containing rostering information.
- Stretched resources that require a workaround now. “We are still waiting for a project, but we’ll just use this form for now, it’s better than nothing.”
- Proprietary data silos which actively prevent information sharing, and
- Paper-based systems where information is recorded once and never used again.
Having disconnected, disparate systems have enormous consequences for delivering integrated patient care.
- There is no single view or source of the truth.
- Providing consistent experiences across like scenarios is impossible.
- There is no capability to analyse what actually happened, what should happen, and what needs to happen in the future.
At best, many ambulance authorities have a common environment to collect and share information, but this is focused on single projects or scenarios, such as finance systems or current Electronic Patient Care Record (ePCR) systems. It doesn’t need to be this way.
What Can Health Learn from Other Industries?
The health sector doesn’t have to start from scratch. We can look to other industries on how they solve similar problems. Building Information Modelling (BIM) has several parallels with healthcare.
BIM is a ‘Digital Twin’ of a physical building and is the process of generating and managing information for a built asset over time. BIM integrates multiple data streams to produce a digital representation of a building across its lifecycle – from planning and design, to construction, operation, and decommissioning. This information can be shared with anyone now, and into the future.
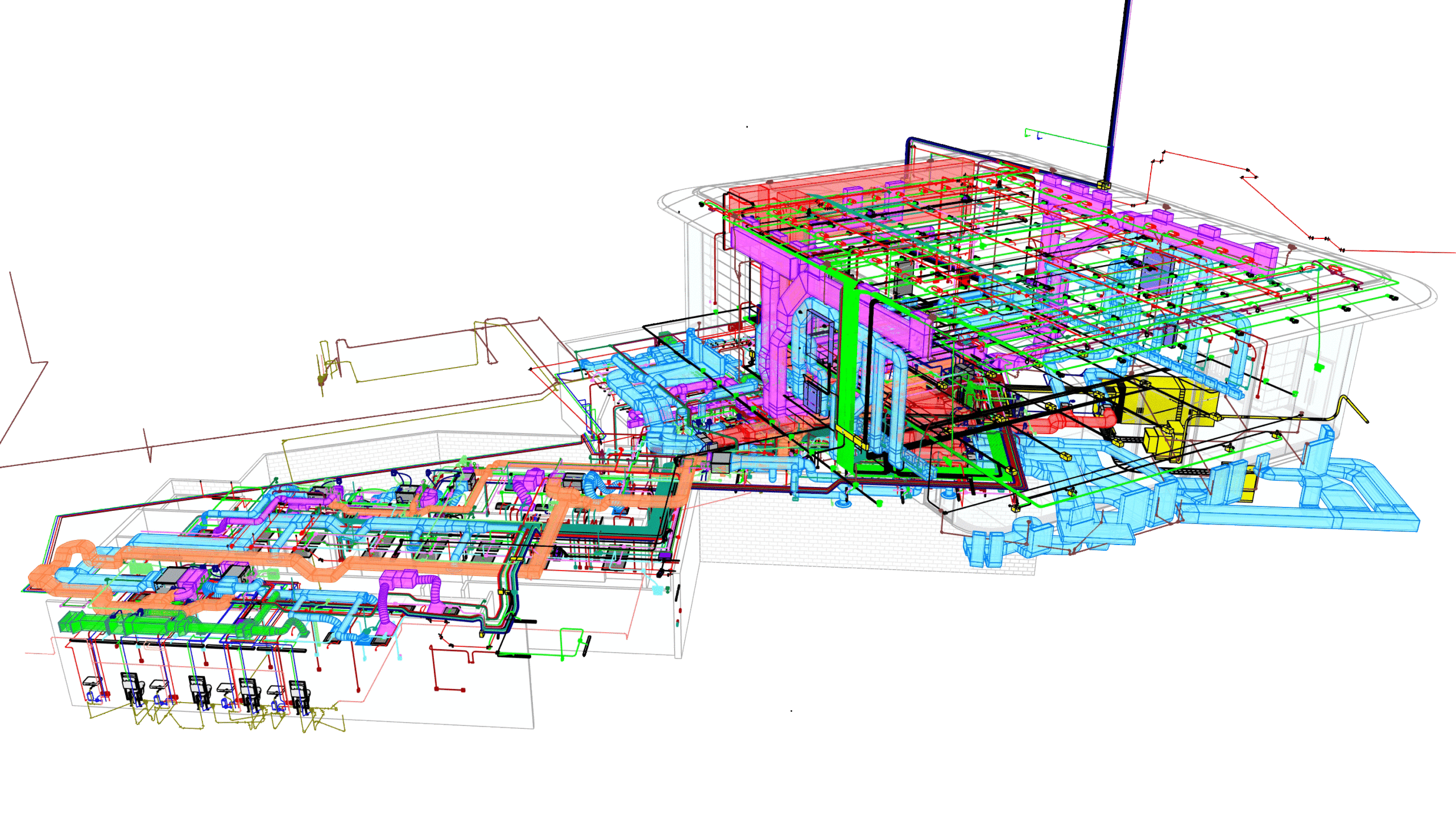
BIM creates more functionality for asset owners, such as:
- Running evacuation simulations.
- Developing costing models, and
- Modelling human behaviour and how people interact with infrastructure use. For example, are there facilities that will never be used?
BIM even provides information for emergency response – for example, how would paramedics access Level 3 from the basement car park? Overall, BIM has provided benefits like cost savings, greater efficiency, and improved communications – all of which can translate into the health space.
The Digital Twins
Terms such as Big Data, Analytics, Data Science, and Data Ingestion are all hot topics, but they all solve one problem – how to represent the physical world in a digital environment.

Otherwise known as Digital Twins, the digital representation of the physical prehospital world is one of the key enablers enabling a truly connected patient journey.
Digital Twins provide new opportunities for information sharing, collaboration, and post-care research. A Digital Twin is a data model that mirrors real life that’s fundamentally open and interoperable. You can leverage it by sharing data in real time with stakeholders and it exists in perpetuity. You have a single view of the truth where cause and effect are modelled and visualised. We can then understand how incidents are related.
These digital representations make the most of stretched resources, eliminates information silos, and creates integrated patient care from the scene to handover at the clinical destination.
What Does Integrated Prehospital Data Mean for Patient Outcomes?
What Does This Mean for Patient Outcomes?
Integrated data within an iPCR system allows for the full visibility of the patient journey – right from when an ambulance is dispatched, to when the patient is handed over to a treatment facility.
For example:
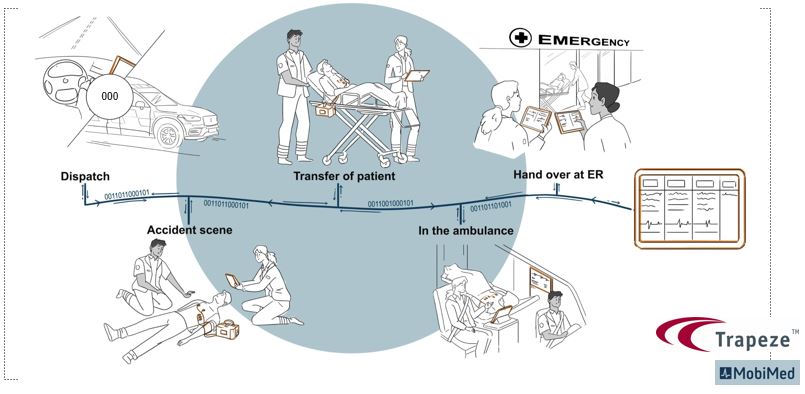
- Ambulance Dispatch: the process starts when an emergency call is received to send an ambulance. All relevant parties know:
- Incident location and access requirements, and
- The patient’s medical history. Paramedics in transit already know a patient’s care requirements.
- At the scene: on arrival, paramedics evaluate the incident and may undertake secondary triage. The dispatch centre receives real-time updates, and the ED is notified. The patient’s doctor is alerted and has provided commentary to paramedics on pre-existing conditions.
- Patient transfer: the patient needs to be transported to a major hospital located 60 minutes away and the crew must conduct a transfer to another ambulance midway. The transporting crew already have access to patient information and are making plans with the receiving ED.
- In the ambulance: crews transfer the patient to the next vehicle seamlessly with no paperwork required. Vitals are being transmitted constantly to the ED.
- ED Handover: the ambulance is received into Bay 3. Intake procedures are completed before reaching the hospital. The patient is transferred directly from the ambulance for immediate treatment.
Other Digital Twin Applications
Having a fully integrated, connected journey is only the beginning for prehospital care. Digital Twins can also be used for:
- Information Sharing: simplifying access to demographic information, national health records and information sharing and analysis.
- Restricted Medication: real-time authorisation and approval requests which can be fully audited and analysed.
- Knowledge Protection: having all data located in one place helps build tacit and collective knowledge, and
- Simulations: providing staff with real-life learning opportunities, e.g., augmented reality to replay incidents.
Conclusion
The applications of Digital Twins in the prehospital space are endless. They eliminate the disconnected information silos and provide a single source of truth for multiple health stakeholders, enabling them to collaborate and help enhance patient outcomes.
The Digital Twins enable a true patient Connected Journey, right from the beginning where an ambulance is dispatched, to patient handover at the clinical destination.
For more information on how Digital Twins can transform your ambulance services, contact us today.
About Corvanta
Corvanta has launched from the former emergency services business within Trapeze.
With a team who are truly dedicated and passionate about what they do, Corvanta understands the impact ambulance services have on people’s lives. In an industry where providing essential health services and excellence in pre-hospital care is paramount, it is crucial patients receive the right care, at the right time, at the right place.
To meet these objectives, our team are solely focused on delivering solutions that connect patient journeys to support meeting KPI’s, improve paramedic safety and influence better outcomes.
For more information, visit corvanta.com



